Diabetic Foot Ulcer Prevention With Diabetes
What is Diabetes?
Diabetes mellitus occurs when there is too much glucose in your blood. This will happen when your body cannot produce enough insulin or is unable to utilise the insulin properly. Diabetic complications can impact many sections of the body including the brain, heart, kidneys and THE FEET.
There are 3 main types of Diabetes mentioned by Diabetes Australia. These include:
- Diabetes Type 1 – an auto-immune condition in which the immune system is activated to destroy the cells in the pancreas which produce insulin. We do not know what causes this auto-immune reaction. More information on type 1 Diabetes is available here.
- Diabetes Type 2 – is a progressive condition in which the body becomes resistant to the normal effects of insulin and/or gradually loses the capacity to produce enough insulin in the pancreas. More information on type 2 Diabetes is available here.
- Gestational Diabetes – Gestational diabetes mellitus (sometimes referred to as GDM) is a form of diabetes that occurs during pregnancy. Most women will no longer have diabetes after their baby is born. However, some women will continue to have high blood glucose levels after delivery. More information on Gestational Diabetes can be found here.
Diabetes increases the risk of developing foot problems. However, you can reduce the risk of any foot and leg problems with daily foot checks and regular foot health assessments and management with our podiatrists at Posture Podiatry.
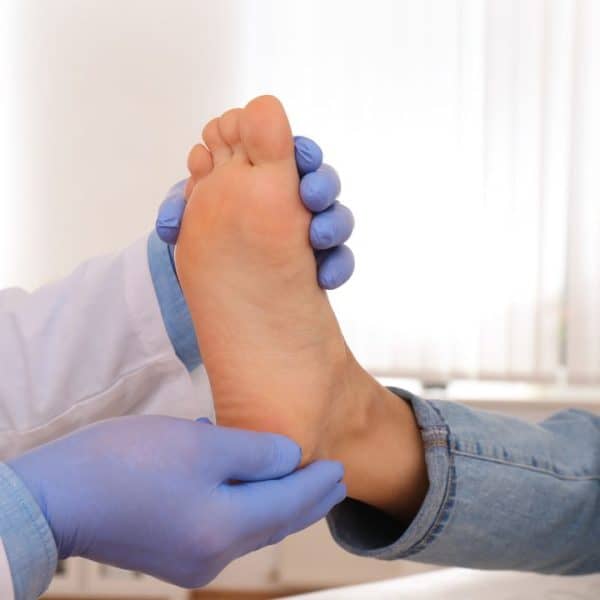
It is imperative to regularly assess the blood supply and nerve sensation in your feet if you have Diabetes. Early detection of reduced blood flow and diminished sensation is absolutely crucial in reducing the risk of foot complications and diabetic foot ulcers.
Your feet are at risk because diabetes can cause damage to the nerves in your feet, blood circulation and increase your risk of infection. Having diabetes can increase your risk of foot ulcers and amputations.
To schedule a diabetic foot examination, call 8362 5900 or
BOOK ONLINE by clicking here
Diabetes Statistics
In 2019, on any given day in Australia, Diabetic Foot Australia (https://www.diabetesfeetaustralia.org/) suggests:
- 50,000 people are living with diabetic foot disease
- 12,500 people are living with a diabetes-related amputation
- Every two hours a person with diabetes has a lower limb removed as a direct result of diabetes-related foot disease
- 80% of diabetes-related amputations are preventable with best practice treatment and on-going management
Diabetes Australia (https://www.diabetesaustralia.com.au/) mentions:
- Every year there are 27,600 hospital admissions in Australia for diabetes-related foot ulcers – many of these admissions end with people having a limb, or part of a limb, amputated.
- More than 4,400 amputations every year in Australia as a result of diabetes and, annually, more than 1700 people with diabetes die as a direct result of foot ulcers and lower limb wounds.
- Diabetes related foot disease costs Australia around $1600 million ($1.6 billion) every single year.
To schedule a diabetic foot examination, call 8362 5900 or
BOOK ONLINE by clicking here
What are the main diabetic foot complications that occur with Diabetes?
Possible diabetic foot complications include:
1. Poor or Compromised Circulation/Blood Supply to the Feet.
Poor diabetic control can cause damage to blood vessels. A reduction in blood supply makes people with diabetes more prone and susceptible to infection as there is a reduced ability to heal
Signs of poor blood supply include:
- Cold feet
- Sharp leg cramps after walking short distances or climbing stairs
- Pain in the feet, even at rest
- Feet looking a different colour, often reddish-blue
- Reduced healing potential, cuts that heal slow
Podiatrists will routinely check the pulses of both feet as part of a diabetic assessment. If the two primary pulses are absent or difficult to detect, Doppler assessment studies may be used if required. Other physical assessments and examination will include colour, temperature, hair growth, skin texture and nail condition. This examination can provide early clues to and help to prevent more serious foot problems. Your podiatrist will also ask various other questions to ascertain whether unusual pain is present (e.g. pain at rest or claudication pain). These may all be signs of poor blood supply.
2. Inadequate Sensation to the Feet.
Nerve damage is commonly referred to as diabetic foot neuropathy and is another complication within our diabetic population. Symptoms result in a loss of sensation and feeling which increases the risk of accidental damage that you may not feel or be aware of (potentially for some time)
Signs of nerve damage include:
- Numbness
- Coldness of the legs and feet
- Burning sensation in the legs and feet, usually at rest
- Tingling or pins and needles sensation in the feet
Your podiatrist has been specifically trained to examine neurological status through various tests including soft touch, monofilament, temperature discrimination, deep sensitivity, vibration and proprioception.
3. Invisibility of the Disease.
In many cases, early signs of Diabetes can go unnoticed. This is because most people don’t feel physically sick in the early stages. The danger then follows; if symptoms are ignored, irregular blood glucose levels can go undiagnosed, which then predisposes individuals to increased severity of the disease. The feet are often neglected until the symptoms become more obvious, by then, often the damage has been done.

Uncontrolled blood glucose levels, poor blood supply and nerve damage are all big concerns for the foot and ankle. Any potential infection can attack the bone (osteomyelitis) and cause a chronic infection in the bones and joints. If an infection isn’t treated at the earliest signs, this could result in diabetic foot ulceration (an infected open sore) and eventually amputation (removal of a toe, foot or limb). It is therefore extremely important to be assessed regularly and check your feet every day!
Other assessments performed by a podiatrist include dermatological (skin and nail assessment), biomechanical examination and general foot care and footwear analysis. (i.e. understanding, self-care and other medical conditions)
To schedule a diabetic foot examination, call us on 8362 5900 or
BOOK ONLINE by clicking here
What can be done to prevent foot problems with Diabetes?
- Maintain appropriate blood glucose levels
- Daily foot care can prevent serious complications
- Know your feet thoroughly; wash, dry and check daily
- Cut your nails straight across
- NEVER attempt at home surgery or self-removal of corns, calluses or ingrown toenails
- Visit your Podiatrist for a regular check-up.
- Avoid walking barefoot in an effort to prevent any skin penetration and foot ulceration
- Have footwear fitted by a professional shoe store. We have a list of shoe stores we can recommend to help you.
- Check for the right length, width and depth of your footwear
- Never wear socks or stockings with tight elastic tops or rough seams
- Exercise regularly and eat a healthy balanced diabetes diet
- Wash your feet daily with mild soap and lukewarm water
- Use a moisturiser after bathing the feet to help prevent cracked heels and skin fissures
- Keep your feet away from direct heat such as heaters, hot water bottles and electric blankets
- Avoid smoking and adhere to recommended alcohol intake limits
To schedule a diabetic foot examination, call 8362 5900 or
BOOK ONLINE by clicking here
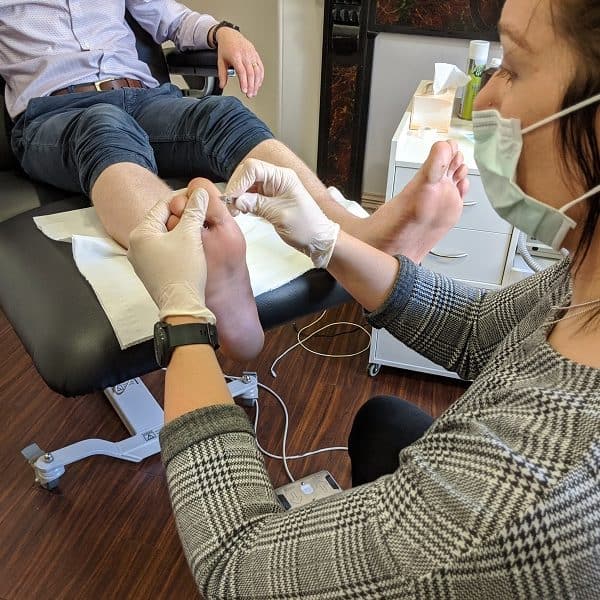
What Happens During a Diabetic Foot Check?
Your podiatrist will examine your feet and assess your gait or walking pattern for any current problems. Following a thorough assessment your podiatrist can better determine your specific treatment needs and how to prevent future problems. In order to do this, our podiatrists will need to:
- Examine the overall condition of your toenails, skin texture, skin appearance, foot structure and foot health.
- The two primary pulses of each foot are checked for normal blood flow.
- Neurological status is checked utilising various nerve checks to ensure there sensation is within normal ranges.
- Footwear will be checked and discussed to ensure shoes are appropriate and fitting correctly.
- Walking pattern is checked to ensure load is evenly distributed with each step throughout the gait cycle. Any uneven load distribution can predispose people to callus formation, pressure lesions and possible ulceration.
How Often Should Feet Be Checked?
Given the seriousness of Diabetes, we advise 6 monthly reviews and monitoring if you are low risk, your Diabetes is well controlled and you have no skin or nail problems. More frequent reviews and management will be needed and recommended if you require more regular foot, skin or nail care or if you fall into the higher risk category.
Always communicate with your Podiatrist and get advice early if you notice any change or problem
If you would like further information or to schedule a diabetic foot examination, call us on 8362 5900 or you can BOOK ONLINE by clicking here.
Further information on diabetes management can be found at:
Health Direct: https://www.healthdirect.gov.au/diabetes
Diabetes Feet Australia: https://www.diabetesfeetaustralia.org/
Diabetes Australia: https://www.diabetesaustralia.com.au/
To schedule a diabetic foot examination, call 8362 5900 or
BOOK ONLINE by clicking here